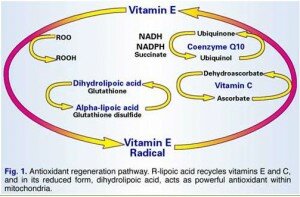
 In researching information about endothelial cell health and function I stumbled across information regarding lipoic acid and cardiovascular health. Sometimes referred to as alpha lipoic acid this vital “co-factor” for enzymatic reactions is critically important for optimizing energy conversion in your mitochondria.
In researching information about endothelial cell health and function I stumbled across information regarding lipoic acid and cardiovascular health. Sometimes referred to as alpha lipoic acid this vital “co-factor” for enzymatic reactions is critically important for optimizing energy conversion in your mitochondria.
What are Mitochondria?
These are the energy factories of your cells and play a huge role in the aging process. At least in theory. First proposed in 1972 by Denman Harman, the mitochondrial theory on aging centers on accumulated damage to the DNA of mitochondria. This leads to increased free radical stress coupled with a decrease in cellular energy production.
So how does this relate to lipoic acid and cardiovascular health?
Researchers have been working to delay mitochondrial aging through a variety of nutrients. One of those nutrients is lipoic acid and the following benefits have been noted:
- Lipoic acid helps to optimize mitochondria function and reverses cell aging.
- Lipoic acid may help to prevent cardiovascular disease, obesity, insulin resistance, and diabetic complications.
- Lipoic acid protects against nerve and brain cell damage.
It was the “may help to prevent cardiovascular disease” that caught my attention. Further investigation led me to a couple of important insights about lipoic acid and cardiovascular health.
The Connection Between Lipoic Acid and Cardiovascular Health!
One of the recent discoveries shows how lipoic acid enhances the effects of insulin. This benefits glucose metabolism by lowering blood sugar levels. This has two potential effects on cardiovascular health. First, it reduces the potential for oxidative stress or damage to the endothelium. Second, it reduces the potential for the pathological cross-linking of glucose and protein to form Advanced Glycation End Products (AGEs). These AGEs have been shown to accelerate many of the aging processes, especially those associated with cardiovascular disease.
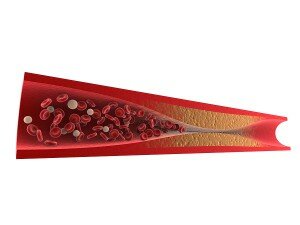
Research is also showing how lipoic acid suppresses the production of inflammatory cell-signaling molecules. This helps to protect the endothelium, which lines all of your cardiovascular system, from plaque formations. It’s these plaque formations that lead to the disease process know as atherosclerosis. Atherosclerosis results in the narrowing of the vascular opening, which leads to an increased risk for strokes and heart attacks.
The following risk factors lead to atherosclerosis: high levels of low-density lipoproteins (LDL or Bad Cholesterol), smoking, high blood sugar levels, and high blood pressure. All of these factors cause direct damage to the endothelium leading to inflammation and the potential for plaque formations.
We’ve already seen how lipoic acid can help reduce high blood sugar levels to prevent oxidative damage to the endothelium. Research also shows how lipoic acid lowers total cholesterol and LDL or bad cholesterol. Both of these actions help to reduce the size and number of potential atherosclerotic plaque formations.
Additionally, lipoic acid enhances the effectiveness of endothelial nitric oxide synthase or eNOS. That’s a long word for the enzyme that the endothelium uses to create nitric oxide – the master signaling molecule of your entire cardiovascular system. Nitric oxide keeps blood platelet cells from sticking together to prevent strokes and heart attacks. Nitric oxide also relaxes the smooth muscle of the vascular wall to keep your blood pressure in a normal range. Thus, nitric oxide is the body’s natural pathway for the prevention of high blood pressure.
When you add it all up, lipoic acid’s antioxidant, anti-inflammatory, and lipid-lowering capabilities make it an ideal nutritional supplement to help protect the endothelium while enhancing the endothelium’s ability to properly produce nitric oxide. All of this results in helping to improve blood flow while reducing the risk for cardiovascular disease. This is why there is a deep connection between lipoic acid and cardiovascular health.
How to Supplement to Obtain the Benefits of Lipoic Acid and Cardiovascular Health!
The consumption of lipoic acid can occur naturally if we choose the right types of food. If you’re looking for animal sources rich in lipoic acid then you need to choose those organs that are high in metabolic activity such as the heart, liver, and kidney. I don’t know about you but I’ve never eaten any of these sources and I don’t ever want to. If you’re not into organ consumption, then steak would be another good option but the leaner the cut the better.
Another alternative is to choose plant based sources like spinach, broccoli, tomato, garden peas, brussels sprouts, and rice bran. These are better food sources since they also help you with other antioxidant properties, which can make a big difference in the aging process.
If you choose to use supplementation to obtain additional lipoic acid then make sure you use the “Right” form of lipoic acid. Lipoic acid comes in what are termed “mirror image” forms labeled “R” and “S.” Only the “R” form is produced and used by the body. However, inexpensive chemical manufacturing will produce equal amounts of “R” and “S” lipoic acid, which is then packaged as either “R/S Lipoic Acid” or “Alpha Lipoic Acid.”
Product manufacturers now have newer precision techniques that allow for the pure “R” lipoic acid to be produced. This has a much higher potency and in many cases it provides twice the active ingredient as you would find in alpha lipoic acid. If you decide to supplement then make sure that you choose a manufacturer that provides you with only the active “R” molecule. This will allow you to use a lower dose and get better results.
A growing trend among cardiac surgeons is the recommendation of lipoic acid and CoQ10 prior to surgery. The thought process is that these two substances help to protect delicate blood vessels during the surgery. The preliminary result has been improved physical and mental quality of life that can last up to a month or more after surgery. Hopefully, these same cardiac surgeons will begin to understand the importance of nourishing the endothelium with the amino acids L-arginine and L-citrulline for improved nitric oxide production and endothelial cell health. This is critically important since the endothelium is involved in wound healing.
If you want to reduce your risk for multiple cardiovascular risk factors then you need to seriously consider lipoic acid. Not only can it be a benefit to cardiovascular health but emerging research shows it to be beneficial to diabetic health, brain health, and a potential anti-cancer help. And, if you want more information on the connection between lipoic acid and cardiovascular health, then I please click here for an article written by the Healthy Fellow.
Together we can work to save a million lives by sharing this information about lipoic acid and cardiovascular health!
Dan Hammer
Dan Hammer has a background in biology, chemistry, and exercise physiology. He used to run one of the largest health club operations in the Chicago area and has been helping people with their wellness issues for more than 25 years.
The information contained in this article is for general information purposes only and never as a substitute for professional medical advice or medical exam. The information about lipoic acid and cardiovascular health has not been evaluated by the Food and Drug Administration and should not be used to diagnose, treat, cure or prevent any disease without the supervision of a qualified medical doctor.


 According to the American Heart Association,
According to the American Heart Association, There is a lot of confusion between arteriosclerosis and atherosclerosis but one thing is certain,
There is a lot of confusion between arteriosclerosis and atherosclerosis but one thing is certain,