 There is a lot of confusion between arteriosclerosis and atherosclerosis but one thing is certain, combined they account for nearly 75% of all deaths from heart disease! This unpleasant statistic comes from the American Heart Association 2004 Heart and Stroke Statistical Update. In the United States alone, approximately 1.5 million heart attacks occur annually.
There is a lot of confusion between arteriosclerosis and atherosclerosis but one thing is certain, combined they account for nearly 75% of all deaths from heart disease! This unpleasant statistic comes from the American Heart Association 2004 Heart and Stroke Statistical Update. In the United States alone, approximately 1.5 million heart attacks occur annually.
The vast majority of these heart attacks are
caused by complications associated with
arteriosclerosis and atherosclerosis.
Most people are familiar with heart attacks or strokes. You likely have a family member or friend who either suffers from the consequences of one or has died due to one. Because of this a great deal of emphasis is placed on preventing heart attacks and strokes. While this is important, the real emphasis should be put upon preventing arteriosclerosis and atherosclerosis because they are the underlying cause of heart attacks and strokes.
To best address this problem we need to clearly define arteriosclerosis and atherosclerosis. Arteriosclerosis commonly refers to those diseases in which the arterial wall thickens and loses its elasticity. Atherosclerosis is one of those diseases. More specifically atherosclerosis refers to the formation of plaque-like deposits consisting of cholesterol and other substances on the arterial walls. These deposits become hardened by fibrous tissue and calcification. This can lead to arteriosclerosis or hardening of the arteries. For simplicity the following definitions will be used:
-
Arteriosclerosis is any disease process that leads to the abnormal thickening and hardening of the arterial walls.
-
Atherosclerosis is the disease process that causes plaque formations to develop on the interior surface of the arterial walls.
Both arteriosclerosis and atherosclerosis cause problems and complication to blood flow. Arteriosclerosis reduces the elasticity of the vascular wall leading to high blood pressure. Atherosclerosis reduces the interior space of the artery leading to reduced blood flow. Reduced blood flow reduces the ability of your cardiovascular system to deliver needed oxygen and nutrients as well as remove waste products from cellular respiration. This then affects the organs’ ability to function optimally.
The most common arteries affected are those in the brain, heart, kidneys, abdominal aorta, carotid artery, and legs. This can then lead to a whole host of symptoms like leg pain, muscular weakness, numbness, cramps, dizziness, chest pain, poor wound healing, and erectile dysfunction.
As atherosclerosis progresses in its narrowing of the arterial space it not only reduces blood flow but it also increases the potential for blood clots to form as well as plaque-like deposits breaking off. This can then cause complete blockages resulting in the common life-threatening diseases we call heart attacks and strokes.
Both arteriosclerosis and atherosclerosis are progressive diseases. This means that they didn’t develop over a short period of time like an infection but they develop over a long period of time. For many in the United States, this disease process can start in early childhood and progressively become more severe as the person ages.
Risk Factors That Can Lead to Arteriosclerosis and Atherosclerosis!
There are certain risk factors that contribute to the development of both arteriosclerosis and atherosclerosis. These risk factors are commonly categorized as “those that can be changed” and “those that cannot”. Here are the risk factors that can be changed:
-
High blood pressure
-
High cholesterol levels, especially LDL cholesterol or low-density lipoprotein cholesterol commonly referred to as “Bad Cholesterol”
-
Cigarette smoking
-
Diabetes
-
Obesity
-
Lack of exercise
-
Western diet, which is excessive in saturated fat from meat, dairy products, eggs, and fast food combined with an inadequate intake in fruits, vegetables, and fish.
These are the risk factors that cannot be changed:
-
Advancing age
-
Being male unless you are a women who has reached menopause.
-
Have a family history of heart disease and stroke especially if it’s based on genetics.
-
African American since this population group has a historically high degree of high blood pressure and diabetes leading to premature stroke, heart attack, congestive heart failure, and death.
As I gathered data for this article many of the websites made the following comment – “The exact cause of arteriosclerosis is not known.”
This author would like to disagree with that statement.
The exact cause of arteriosclerosis and atherosclerosis is known!
It is damage to the endothelial cells that line all of your cardiovascular system which reduces their ability to properly produce nitric oxide, the master signaling molecule of the cardiovascular system.
We will examine this statement and the standard treatment programs used for these cardiovascular diseases in our next article entitled “Arteriosclerosis and Atherosclerosis – Treatment Programs!”
Together we can work to save a million lives!
Dan Hammer
Dan Hammer has a background in biology, chemistry, and exercise physiology. He used to run one of the largest health club operations in the Chicagoland area and has been helping people with their wellness issues for more than 25 years.

 Many in the health care profession have forgotten about the positive relationship between niacin and cholesterol. Instead they have promoted
Many in the health care profession have forgotten about the positive relationship between niacin and cholesterol. Instead they have promoted  If you read my post
If you read my post  Cholesterol reduction through the use of statin drugs has become a big and profitable business for the pharmaceutical industry. As more and more people have opted for a pill to help control their cholesterol levels fewer people are using fiber as their first line of defense. If you read my blog post
Cholesterol reduction through the use of statin drugs has become a big and profitable business for the pharmaceutical industry. As more and more people have opted for a pill to help control their cholesterol levels fewer people are using fiber as their first line of defense. If you read my blog post 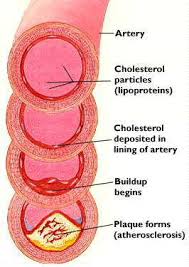
 Happily Married or Headed for Divorce?
Happily Married or Headed for Divorce? When people think of heart disease they rarely think about the endothelial cells that line all of your blood vessels. Most people usually associate heart disease with the heart or with problems in their circulatory system. While both of these can be major contributing factors in heart disease, for most people it is the health of their endothelial cells and their ability to properly produce
When people think of heart disease they rarely think about the endothelial cells that line all of your blood vessels. Most people usually associate heart disease with the heart or with problems in their circulatory system. While both of these can be major contributing factors in heart disease, for most people it is the health of their endothelial cells and their ability to properly produce